Role of Stem Cells in Immediate Reconstruction by Bone Graft after Radical Resection of Malignant Tumors of the Jaw, Clinical and Experimental Studies
Raja Kummoona*
FRS med, FDSRCS, FICD, Emeritus professor of Maxillofacial Surgery, Iraqi Board for Medical Specializations, Baghdad, Iraq
Corresponding author: Raja Kummoona, FRS med, FDSRCS, FICD, Emeritus professor of Maxillofacial Surgery, Iraqi Board for Medical Specializations, Baghdad, Iraq
Citation: Kummoona R. Role of Stem Cells in Immediate Reconstruction by Bone Graft after Radical Resection of Malignant Tumors of the Jaw, Clinical and Experimental Studies. Genesis J Surg Med. 4(2):1-09.
Received: November 15, 2025 | Published: December 10, 2025
Copyright© 2025 Genesis Pub by Kummoona R. This is an open-access article distributed under the terms of the Creative Commons Attribution 4.0 International License (CC BY 4.0). This license permits unrestricted use, distribution, and reproduction in any medium, provided the original author(s) and source are properly credited.
DOI: https://doi.org/10.52793/GJSM.2025.4(2)-40
Abstract
Role of stem cells in immediate reconstruction of the mandible by bone graft was quite interesting in cases with malignant tumors after radical resection of the tumors.
Stem cells derived from mesenchymal tissues. IN this study we observed strong relation between mesenchymal stem cells with bone graft. the stem cells were derived from the bone marrow of the resected mandible, periosteum and overlying muscles.
We reported few cases with malignant tumors of the jaw were managed by immediate reconstruction of the mandible by bone graft. The aim was to prevent mutilation, deformity of the face and to restore normal masticatory function of the jaws.
Immediate reconstruction by bone graft was to achieve normal shape and contour of the jaw and to prevent psychological trauma and frightening from malignancy from the patient.
We did practice this type of surgery for years and decades. Failure of bone grafting were noticed by new specialists were considered as hambling surgery. Also, failure of bone grafting was occurred with patients receiving DXT or chemotherapy. Its contra indicated to do bone grafting fore cases received DXT and chemotherapy.
Keywords
Stem Cell; Immediate; Reconstruction; Lower Jaw; Bone Graft; Malignancy.
Introduction
Bone grafting became very interesting for reconstruction of bones defect after cancer surgery. We did notice very few people practicing bone grafting for this type of difficult surgery.
Bone grafting is a difficult task to approached by new surgeon because lack of knowledge, skill and expertise, once they practice this kind of surgery, they faced usually failure of grafting cases within few weeks the cases showing infection and rejection of the graft. Hambling surgery no more accepted now adays.
People frightening from cancer because it may end with death. The survival rate in orofacial region in the best cases was 5 years and 10 years for complete remission but the author reported recurrence of oral cancer after fifteen years. Head and neck cancer was reported as 8% of the total body malignancies including orofacial, salivary glands tumors, parotid, oropharynx, orbit, jaws and skin.
The majority of oral tissue were affected by squamous cell carcinoma while other varieties of cancer were derived from mesenchymal tissue. Tumors such as fibro sarcoma, osteogenic sarcoma, rhabdom myo sarcoma, Kummoona jaw lymphoma, Burkitt’s Jaw lymphoma and non-Hodgkin’s and Hodgkin’s lymphoma.
Basal cell carcinoma affecting the skin of the face due to lack of melanin in the skin of white people exposed to sun light. This type of cancer locally invasive but does not do metastasis to cervical lymph nodes unless it’s converted to squamous cell carcinoma.
Oncogenic viruses were considered as strong cause of cancer. EBV virus proved to be the causative virus of jaw Burkitt’s Lymphoma and also causing nasopharyngeal carcinoma and infectious mononucleosis. Herps like viruses causing Kummoona Jaw Lymphoma. It was reported that herpetic papilloma virus was associated with oral cancer as reported by Harvard few years ago. We have not to exclude Depleted uranium as a strong cause of aggressive type of Oral cancer in south of Iraq after invasion of the country.
Materials, Method and Results
Several cases reported were treated by radical resection of malignant tumors of lower jaw with immediate reconstruction by bone graft. The majority of surgeons they do don’ts advice reconstruction by bone graft because they may face difficulties to do that but they do reconstruction by prosthesis an easy and quick way to avoid possibility of recurrence and for future treatment by DXT and chemotherapy.
Our technique based on idea that if we can remove the whole malignant tumors from the jaws, we should proceed to do that, because by radical resection of malignant tumors without remanent of malignant cells. By this technique we can avoid severe deformity of the jaw and face and complication of chewing foods and to avoid psychological illness of patients especially young patients.
In the beginning of bone grafting, it was a gambling technique for us and we don’t know how much we are successful in this type of surgery.
Our aim was directed to study the role of mesenchymal stem cells in bone grafting derived from stump of the resected part. We prefer to do immediate reconstruction of the mandible by bone graft before giving DXT or chemotherapy to the cancer patients. Once the patients were received DXT or chemotherapy there were no chance of bone grafting success, because its effect on tissues and induces Atheros sclerosis.
We prefer to use the iliac crest because the graft was taken from iliac because of bulk, thickness as cortical- cancellous bone graft, its vascularity, the shape and curvature of the graft was required to fit the defect of the mandible. We have to measure the defect to know the length of the graft to be taken. The Iliac crest considered as the best Bank of bones, there are few varieties of bone graft from iliac crest either as cortical cancellous bone graft, BI cortical bone graft or as cancellous bone graft as chips or mesh usually used to enhance healing of delayed healing of fractures bones.
We did use previously Kummoona Chondro-Osseous graft for reconstruction of temporomandibular joint in ankylosed type for restoring growth and function of the jaws and midface in children.
Bone graft was used also for reconstruction of the mandible in post- traumatic missile war injuries for people lost part of their jaw as an elective surgery. (Figure 1, Figure 2).
Figure 1A: Photo of bone grafting of lower border of mandible of Rabbit.
Figure 1B: X-ray of Rabbit mandible after 3 months showing good healing of bone graft.
Figure 2: Photograph showing the histology of bone grafting and mesenchymal stem cells on the border as dark dots, the lower photo showing the good cellular changes of the bone graft and stump of the mandible with no difference between the graft and mandible in presence of osteoid tissue.
Technique of Bone Grafting
We exposed the whole iliac crest from posterior to anterior crest from lateral side to avoid perforation of the colon and viscera in medial side. Also to avoid damages to lateral cutaneous nerve.
The iliac crest was splatted by horizontal way by osteotome of 8mm and width a width of about 5 cm, the graft was taken as one piece. The resected part should be measured. The graft split from posterior crest forward to anterior crest. The graft be removed carefully with good handling as one piece to avoid fracture of the graft. Once the graft was shorter than the defect, we can add graft from medial side of iliac crest. The two pieces joined and fixed firmly to each other with decortication of both pieces was required before fixation. (Figure 3, Figure 4, Figure 5).
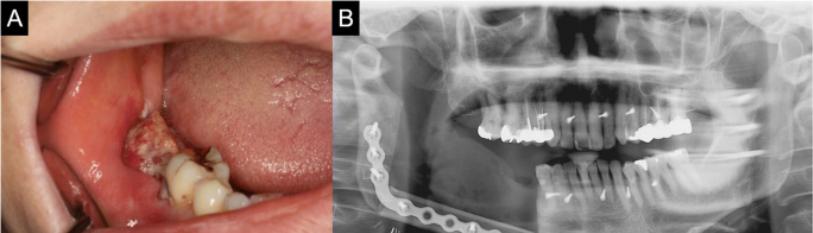
Figure 3A: Fifty years lady with extensive malignant Ameloblastoma of left side of the mandible.
Figure 3B: X-ray of posterior-anterior view showing destruction and osteolytic changes and resorption of bone in the ascending ramus and body of the mandible.
Figure 3C: Photo showing immediate bone grafting after radical resection of malignant ameloblastoma.
Figure 3D: Resected specimen of Ameloblastoma.
Figure 3E: Posterior-Anterior view of X-ray showing excellent healing of bone grafting.
Figure 3F: Photo of the patient without any deformity after 4 years.
Figure 4A: Young female patient of 17 years of age with extensive Rhabdo—myosarcoma of the left side of the mandible.
Figure 4B: Lateral oblique of left lower jaw showing sever destruction and osteolytic changes.
Figure 4C: Radical resection of highly malignant Rhabdo-Myo sarcoma of the mandible.
Figure 4D: Bone grafting immediately after radical resection of the tumors.
Figure 4E: Posterior-Anterior view of X--ray showing excellent bone grafting after 6 months.
Figure 4F: photo of the patient after six months with excellent face profile.
Figure 5: Composite photo graph showing post-traumatic of missile war injuries by high velocity rifle bullet, six months later we did remove the scar and reconstructed the area by Kummoona Lateral cervical flap again after six months we did reconstruction of the mandible by bone graft and photo of the patient after one year.
Experimental Studies
Experimental studies were done by using Rabbits as experimental model to study the cellular changes that occurred between stump of bone and bone graft.
Twelve of Young Rabbits of 3 months of age were used in this study, were divided into two groups, each group of 5 Rabbits as group A and group B. Two Rabbitts were used as control.
Sub mandibular incision was used for dissection and for exposing the lower border of the mandible of the Rabbit, one cm was resected from lower border and a piece of 2 cm of bone graft was harvested from iliac crest of the same Rabbit. We applied Surgical of regenerated cellulose on the graft in one group B only. The graft was fixed firmly by stainless steel wire of 0.25mm. Before fixation we did decortication of both graft and stump of the Rabbit mandible to get maximum contact between the graft and body of the mandible. This technique was applied on 10 Rabbits. Two Rabbitts were left as control.
The Rabbits were left in their colony for 3 months and terminated after that. Resected part of stump bone of the mandible and graft as specimens were immersed in buffer formaldehyde of 10% for ten days with decalcified solution, slides prepared for H&E staining.
Histopathological Studies of Bone Grafting
The histology of bone grafting was quite interesting, showed formation of clot, plat less aggregation with releasing plat lets growth factor (PGF), healthy granulation tissue formed and mesenchymal stem cells were derived from bone marrow of the mandible, periosteum and covering muscles. Formation of fibroblast and chondrocyte were also observed. We did find no differences in healing process of bone graft between group A and group B. We thought that surgical might enhance healing process of the bone graft. (Figure 3, Figure 4).
This experiment was aimed to study the viability of bone grafting and the cellular changes that occurred and associated between the bone graft and stump of the mandible. (Figure 1, Figure 2)
These bone grafting was not only applied in tumors resection, but also was used for reconstruction of the mandible in cases with post-traumatic missile war injuries 6, and it was very successful in our hands for reconstruction of maxilla and bone grafting was used in Road traffic accident for reconstruction of frontal bone, orbits and zygoma.
References
- Kummoona R. (2018) Bone grafting recent advances with special reference to Craniomaxillofacial Surgery. Book, Ed Raja Kummoona. Intch Open access.
- Kummoona R. (2020) Missile war injuries of Craniofacial region Craniofacial Surg. 1307-1311
- Kummoona R et al. (2018) Reconstruction of Lower Jaw by iliac bone graft, experimental studies on Rabbitts and role of mesenchymal stem cell. J of Stem Cell Regenerative Biology. 4(1)20-24
- Kummoona R. (2018) Bone Grafting Recent advances with special references to Craniomaxillofacial Surgery. Book, Ed, Raja Kummoona. In Tech Open.
- Kummoona R. (2017) Kummoona Chondro-Osseous graft good substitute to condylar growth center and for correction of facial deformity in children. Arch Otolaryngol Rhinol.3(3)98-102
- Kummoona R. (2021) Management of Missile War Injuries. Book, Ed, Raja Kummoona. Index of Sci.

